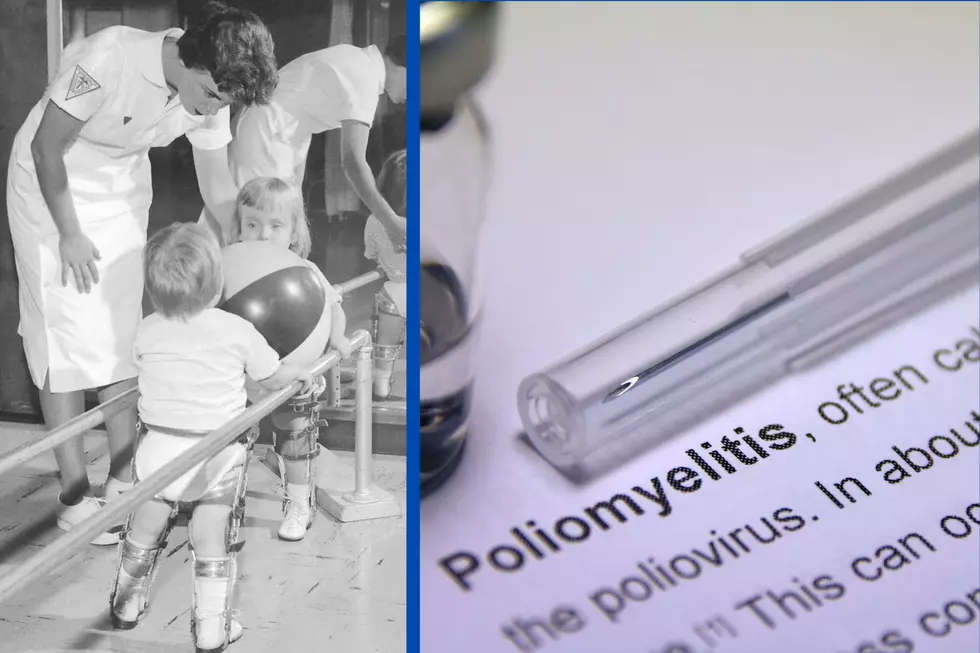
Country’s first known polio case in years is in NY: What NJ needs to know
New York has confirmed a case of polio in the Hudson Valley region, the first to arrive in the U.S. in about a decade.
The Rockland County case confirmed by New York state health officials was in a young adult who began experiencing weakness and paralysis about a month ago, as CNN reported on Thursday.
While no case of polio has originated in the U.S. since 1979, the virus has been brought into the country by travelers with polio — some of whom might be asymptomatic but spreading the virus.
So how concerned should New Jersey's general public be?
Not very, if they have followed the CDC guidance for immunizations.
There is no cure for polio. Polio vaccine is the only protection against the virus.
Before vaccines were available, polio was once one of the most feared diseases in the U.S. In the late 1940s and early 1950s, polio outbreaks caused more than 15,000 cases of paralysis each year, according to the CDC.
Inactivated polio vaccine (IPV) has been the only form of the vaccine that has been given in the U.S. for more than 20 years — by shot in the leg or arm, depending on the patient’s age.
Oral polio vaccine (OPV) has still been used in other countries, even after being discontinued in the U.S. since 2000.
Vaccine-derived poliovirus (VDPV) is a strain of the weakened virus initially included in the oral vaccine — which in some cases changes over time and behaves more like the naturally occurring virus.
This means it can be spread more easily to people who are unvaccinated against polio and who come in contact with respiratory secretions, like a sneeze, or fecal matter of an infected person — including through contaminated wastewater.
Cases of such oral vaccine-associated paralytic polio (VAPP) have been recorded this year in other countries — including in London, United Kingdom, in June and in Israel in April.
In 2013, an infant who had received the oral vaccine in India and was severely immunocompromised wound up developing polio and dying while in the U.S., according to the CDC.
Between two and 10 out of 100 people who have paralysis from polio infection die, according to federal health officials, because the virus affects muscles that help them breathe.
Even children who seem to fully recover can develop new muscle pain, weakness, or paralysis as adults, 15 to 40 years later — which is called post-polio syndrome.
School-aged children and polio risk
The polio vaccine continues to be included on the CDC standard child immunization schedule and also is part of the required school immunization schedule for all children.
That means school-age children are vaccinated before they start school in this country, unless guardians avoided the requirement, such as with medical exemptions.
The Centers for Disease Control and Prevention estimates that about 1 in a million doses of the polio vaccine causes an allergic reaction.
Children in the U.S. are advised — and required to attend school — to get four total doses of inactivated polio vaccine (IPV), with one dose at each of the following ages:
— 2 months old
— 4 months old
— 6 through 18 months old
— 4 through 6 years old
Adults and polio risk
Most adults do not need polio vaccine because they were already vaccinated as children — though the following groups of adults are at higher risk:
— Healthcare workers treating patients who could have polio or have close contact with a person who could be infected with poliovirus.
— Adults traveling to a country where the risk of getting polio is greater.
— Adults working in a laboratory and handling specimens that might contain polio virus
Adults who are at increased risk of exposure to polio and who have previously completed a routine series of polio vaccine can receive one lifetime booster dose, according to the CDC.
Erin Vogt is a reporter and anchor for New Jersey 101.5. You can reach her at erin.vogt@townsquaremedia.com
Click here to contact an editor about feedback or a correction for this story.
LOOK: What are the odds that these 50 totally random events will happen to you?
Gallery Credit: Isabel Sepulveda
Beautiful sunflower fields to visit in NJ 2022
Gallery Credit: Erin Vogt
UP NEXT: See how much gasoline cost the year you started driving
UPDATE 2024: All NJ stores that sell legal cannabis
Gallery Credit: Erin Vogt
Netflix’s Most Popular English-Language TV Shows Ever
More From New Jersey 101.5 FM